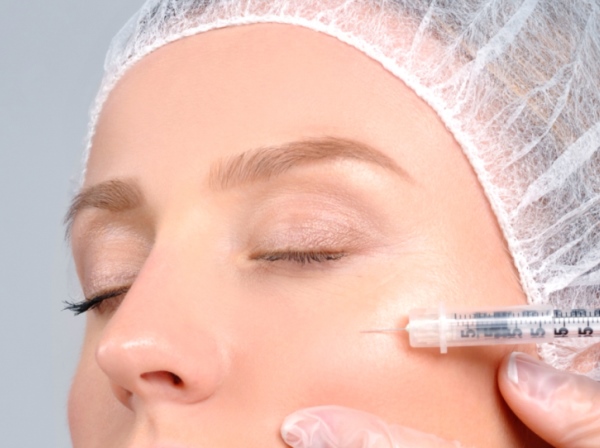
Australian woman has been left permanently blind in one eye after having a cosmetic filler injected at a Sydney beauty clinic.
Although over 100 cases of permanent blindness from cosmetic fillers have been reported around the world in recent years, including one in New Zealand last March, it is the first such case reported in Australia.
The “tragic case” was brought to light at the 2018 Non-Surgical Symposium held by the Australasian Society of Aesthetic Plastic Surgeons (ASAPS), the Cosmetic Physicians College of Australasia (CPCA) and the Australasian Society of Cosmetic Dermatologists (ASCD) on the Gold Coast last month.
During a panel discussion at the conference it was revealed that the woman attended the Sydney clinic to “improve the shape of her face” but just hours later was declared legally blind in one eye.
A delegate told Professional Beauty that the woman had an adverse reaction to an injection of hyaluronic acid filler and was therefore taken to a hospital for treatment.
The delegate said the cosmetic nurse injector did not inject hyaluronidase into the affected area in an attempt to reverse the effect as her supply was out-of-date ‒ when injected within 90 minutes hyaluronidase dissolves hyaluronic acid and reverses any blockages.
The woman was declared legally blind at the hospital.
Although unable to confirm or discuss the details of the case, ASAPS president Dr Mark Magnusson says that “even in the most experienced hands, the risk of having filler treatments should not be underestimated”.
“The risks are very much real.”

He says the three most dangerous risks are “blindness, stroke and skin death (skin necrosis)” but other possible complications and side effects include infection, foreign body granuloma, hypersensitivity, painful lumps, bio fill formation resulting in chronic infection and irritation, skin discolouration and pigmentation, numbness, and hypersensitivity due to nerve irritation.
And although the Sydney tragedy is Australia’s first reported case of blindness caused by cosmetic filler, Assoc Prof Mark Magnusson is certain it won’t be the last.
“There has been an explosion of operators moving into the cosmetic industry,” he says.
“The de-medicalisation of non-surgical cosmetic treatments have trivialised them. The marketing experts have succeeded in convincing the public that these procedures are easy, convenient and can be accessed in a ‘drive-through’ manner with no downtime. The decline in standards has resulted in a compromise to patient safety.”
The filler injection in the Sydney case was performed by a qualified practitioner, but Assoc Prof Magnusson says “the regulations that cover the administration of fillers leave it wide open for a range of people to prey on people’s vulnerabilities offering cut-price treatments”.
“Creative marketing strategies and aggressive sales tactics have muddied the waters and sadly patient safety has been forgotten despite the risks being real.
“These marketing tactics lure people in on the premise of achieving their desired aesthetic goals but often the cost savings result in an inferior result and greatly increase the risks to patient safety.”
“Unfortunately under the current regulation there is no way for a patient to fully known the risks involved without their own background research. They also have no idea of working out if the practitioner is a well-trained expert or a novice who is training on the job.”

Nicole Montgomery, a cosmetic surgery nurse and founder of Trusted Surgeons (an online platform that helps individuals considering cosmetic procedures “make safe, informed and educated decisions”) also believes that another case of blindness by filler is inevitable.
“It’s bound to happen again,” she says.
Montgomery says Trusted Surgeons is regularly inundated with calls for help from men and women around Australia who are suffering emotionally and physically from botched filler injections.
She has seen “lots of minor complications that can be problematic such as asymmetry, bruising, skin breakouts and nerve damage leading to paraesthesia or numb areas of the face” as well as “many cases of infected filler requiring surgery”.
In addition “people are also often be left looking odd or weird looking when too much filler is used by the untrained hand”.
Montgomery believes that Australia’s lack of industry regulations will ensure that such poor patient outcomes continue to occur.
“With the market being so lucrative, there is always an influx of inexperienced injectors that have access to doctors via Skype to get the scripts required to inject.
“Until the industry is regulated and there is minimum standards for injectors, including education standards and where the injections can take place, there will be no change to the dangers unsuspecting people will face.”
She says the best way for consumers to avoid such risks is to do their homework and “ask lots of questions”.
“Your injector should be a doctor or nurse injector with a doctor close by that has extensive knowledge of the face and its structures.
“…if your injector is setting up on a kitchen table prior to injecting you – alarm bells should be going off.
“These non-surgical treatments should be done in proper medical practices that have the appropriate safety equipment and procedures in place.
“If you’re Skyping a doctor in another state (more alarm bells) then chances are medical help is not close by in case of an emergency.
“Ask your injector about their qualifications and the last conference they attended to keep their skills up. Ask about the filler that is being used and what filler is used in different parts of the face. The more knowledge your arm yourself with the better.
“This will help minimise your risk of suffering any major complications such as blindness.”
“Of the 100 or so cases reported worldwide, there has not been a case where the patient has had total vision restored post trauma.
“Now with the first reported case in Australia, it is imperative that everyone is cautious and makes appropriate and well informed decisions around cosmetic injectables.”